It has been established through laboratory, field and animal experiments that there is a relationship between exposure to noise and cardiovascular diseases, such as ischemic heart disease and hypertension. In particular, a number of studies have shown that exposure to intense noise affects the sympathetic and endocrine system increasing heart rate, blood pressure, peripheral vasoconstriction, and stress hormones [3]. These effects do not only occur in waking hours but also during sleep.
Other effects of noise that have also been reported in subjects exposed to high levels of noise are the release of stress hormones (including adrenaline, noradrenalin, and cortisol).
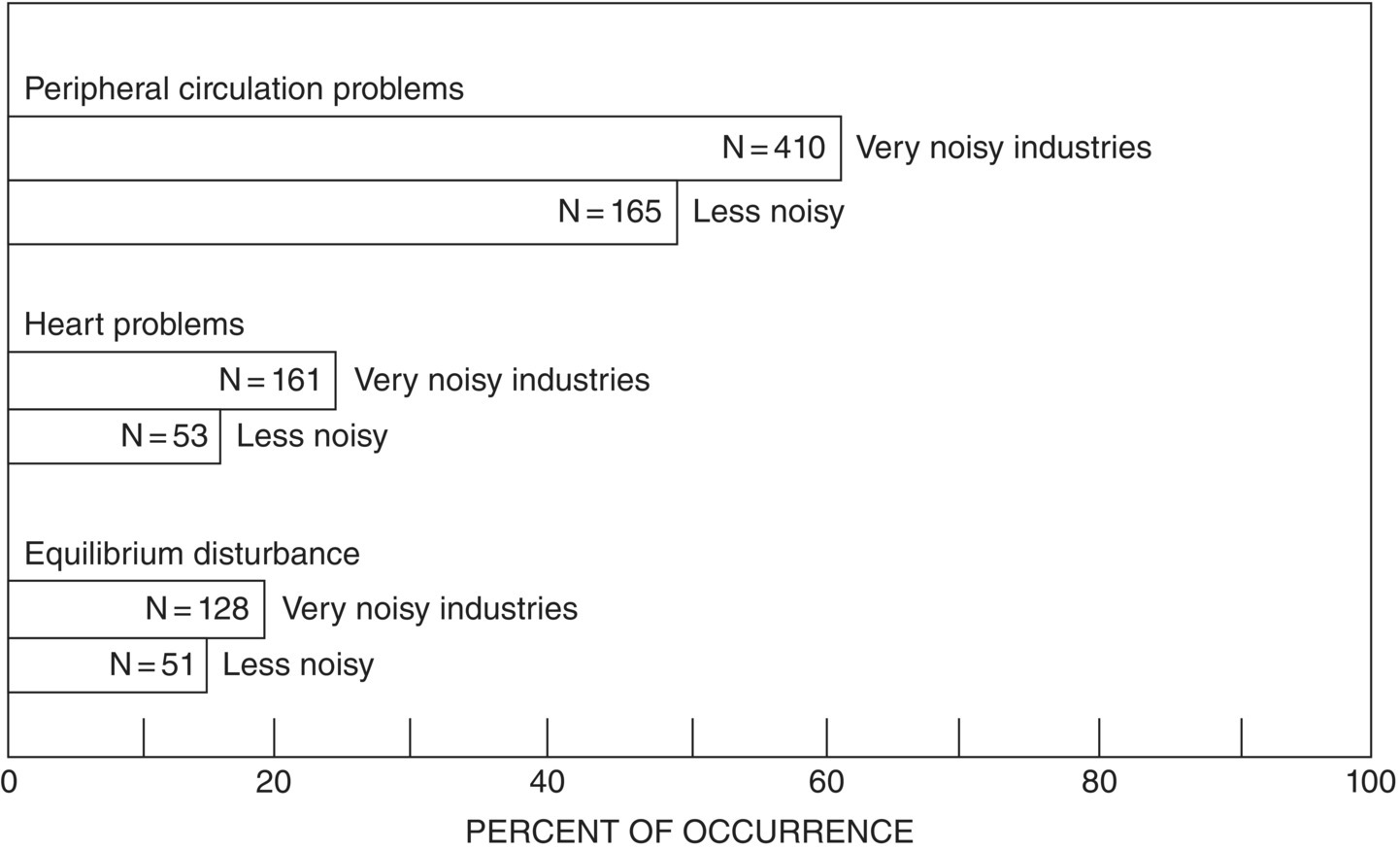
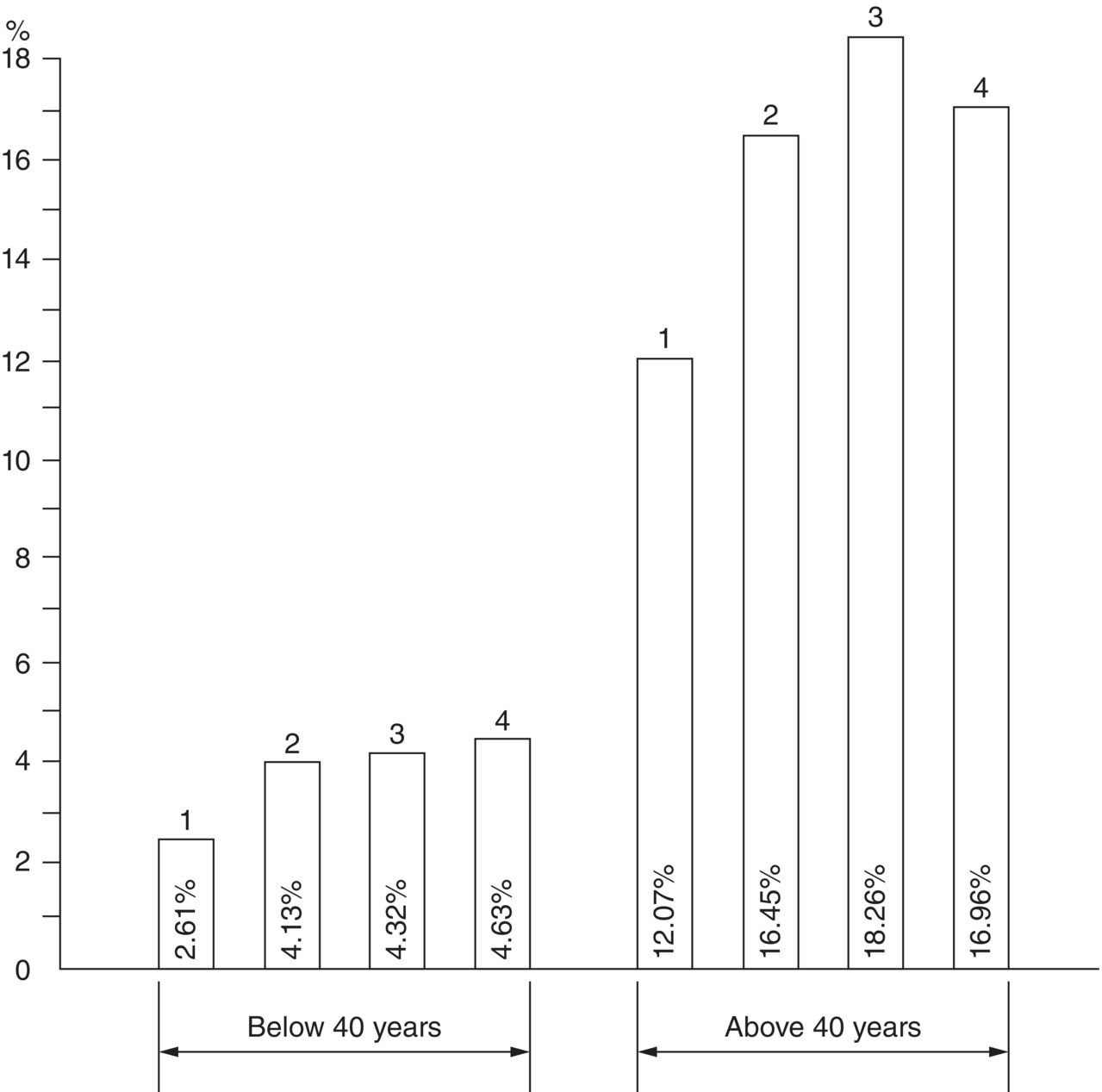
We may define stress as a state of arousal which can eventually have adverse health effects. The general response to any form of stress is called the adaptation syndrome. This consists of three states: alarm, a stage of resistance, and a stage of exhaustion. Miller [2] suggested that it is unlikely that any long‐term stress effects are produced unless noise levels are sufficient to produce hearing damage and loss. However, some studies have been published which suggest that in some industrial situations noise‐induced stress can produce adverse health effects. Figure 5.1 shows the result of an early study by Jansen [4] on 1005 German industrial workers and Figure 5.2 shows the incidence of hypertension in male and female workers in noisy workshops after Andriukin [5]. As Kryter [6, 7] pointed out, however, these results could be misleading. In the noisy environment other factors may be important such as poor ventilation, heat and light, danger from accidents, anxiety over job security, and the possible selection of people with lower general health and economic or social status for intense‐noise jobs. More recent epidemiological studies carried out in the occupational field have shown that employees working in noisy environments are at a higher risk of high blood pressure and myocardial infarction. It has been observed that workers exposed to A‐weighted noise levels greater that 75 dB reported statistically significant increases in blood pressure [8].
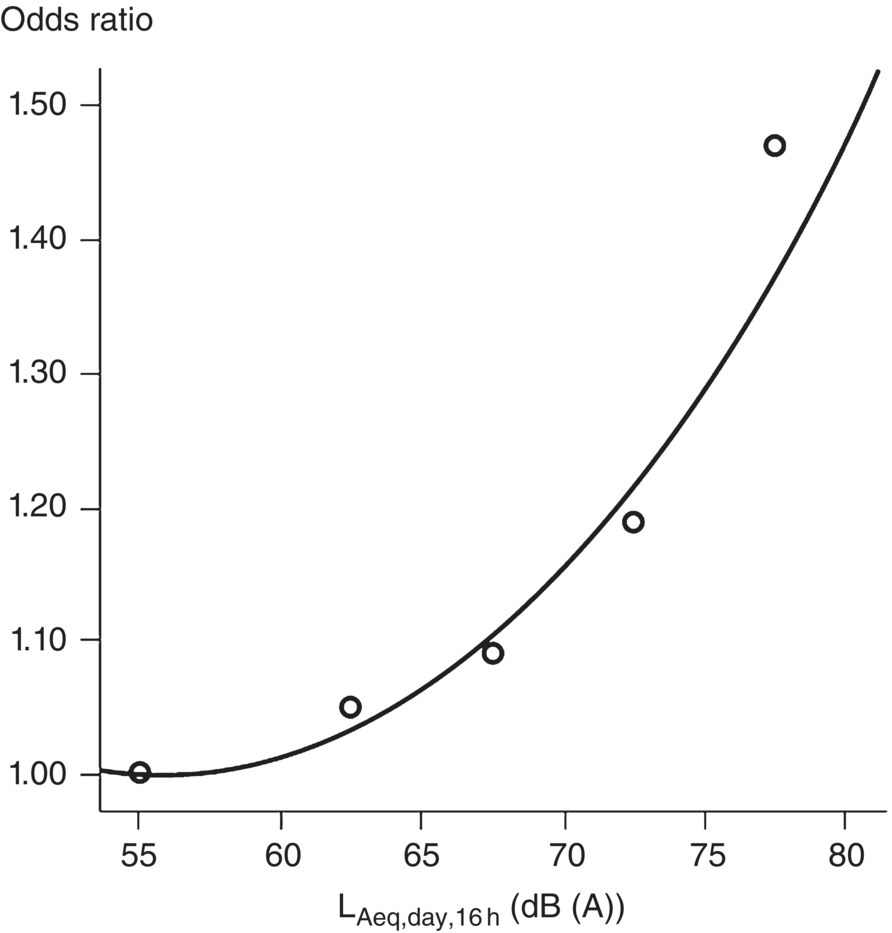
Based on a meta‐analysis Babisch [9] reported the relationship between road traffic noise and cardiovascular risk. As shown in Figure 5.3, a cubic exposure‐response function is given for the increase in relative risk (odds ratio) per increment of the noise level measured as an A‐weighted average noise exposure over a 16‐hour daytime period, Leq,16h (see Chapter 6). Since this relationship was based on different studies with different A‐weighted noise level ranges, it was suggested to use Leq ≤ 60 dB as a reference category (relative risk = 1). For example, the relative risks for subjects who live in areas where Leq is between 70 and 75 dB would then approximate to 1.15 and 1.29, respectively. A similar study was recently published on the exposure‐response relationship of the association between aircraft noise and the risk of hypertension [10].
Mixed epidemiological evidence has been reported for effects of noise on coronary heart disease and coronary risk factors in adults. Clark and Stansfeld [11] have attributed this fact to the difficulty of performing objective measures of blood pressure and to confounding factors associated with coronary heart disease that are difficult to isolate during research. Usually the blood pressure has been estimated indirectly through self‐reported measures of hypertension and antihypertensive drug use in many epidemiological studies. However, a unique study recently performed in Europe [12] used reliable measures of blood pressure in the analyses. The research was performed on individuals who had lived near to one of six major airports for five years or more. The study found increased risk of hypertension related to long‐term noise exposure, for both nighttime aircraft noise and daily average road traffic noise.
Leave a Reply